By Ky Wynne, Physiotherapist at Lifecare Prahran Sports Medicine.
Muscle injuries are one of the most widespread injuries sustained during sporting activity.
Across several professional sports, acute muscle injury makes up a whopping 23% to 46% of all injuries – when you think about it, this is a huge percentage. [1, 2, 3]
Generally hamstring strains and/or tears are the most common muscle injury, while adductors, quadriceps, and calf injuries closely follow in prevalence.
Injury rates vary depending on the sport and the demands of that sport.
A great example here would be sprinting, sprinting involves rapid acceleration and deceleration which places high strain on the hamstrings, thus making this the most common sprinting injury, whilst movements associated with change of direction place higher strain on the adductors (groin), so you will see these types of injuries in games of footy.
Males generally have a higher incidence of muscle injuries, often thought to be due to the higher-intensity of running and sprinting taking place [1], again these rates vary between sports and the use of different muscles.
The end-to-end muscle process
All muscle injuries undergo similar physiological changes, with early muscle damage and inflammation occurring first, followed by regeneration and renewal of the muscle fibres [3].
See figure-1 below for a more detailed step-by-step breakdown.
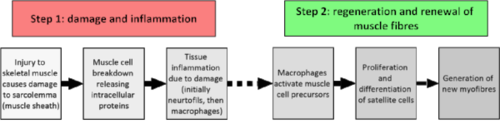
Figure-1
A comprehensive assessment
The assessment and diagnosis of a muscle injury should be completed by a physiotherapist or trained medical professional.
Typically the injury incident will point towards a muscle strain, with jumping, running, change of direction and kicking all common causes.
The examination of the injury will vary depending on the muscle and area involved, however tests will often include:
- Palpation of the muscle and surrounding areas
- Muscle strength assessment
- Muscle length tests
- Functional movements
- Assessment of other areas to rule out different pathologies or injuries
Imaging, like magnetic resonance imaging (MRI) or ultrasound, is often not required unless the injury is of a more severe nature.
However, it can assist the therapist in determining the grade of injury and the healing time frames needed before the individual can return to play.
What treatment is in store for you?
Treatment involves a number of stages, which includes an early acute phase, followed by rehabilitation and then a graded return to sport.
While not appropriate for every situation, as a whole, earlier assessment and commencement of a treatment plan will improve outcomes and will allow the individual to return to activity sooner [3, 4].
Many individuals return to activity or sport when pain resolves and without finishing a full course of rehabilitation; increasing the risk of re-injury.
Re-injury post return to activity is a significant risk, especially following hamstring strain [4].
Due to the high rates of subsequent injury, completing a thorough return to sport assessment following rehabilitation is recommended to determine if any deficits still exist in strength or function.
Prevention is key
Prevention of muscle injury is also important to consider.
While you can never 100% prevent against muscle damage, completing targeted prehabilitation programs can substantially reduce the chance of injury.
If you have suffered a previous injury (especially a muscle strain), completing a comprehensive assessment and targeted exercise program will likely have significant value.
If you want to prevent the occurrence of muscle injury or have faced injury before and want to lower the risk of re-injury, book in an appointment with your local Lifecare physiotherapist.
References
- Feeley, B. T., Kennelly, S., Barnes, R. P., Muller, M. S., Kelly, B. T., Rodeo, S. A., & Warren, R. F. (2008). Epidemiology of National Football League training camp injuries from 1998 to 2007. The American journal of sports medicine, 36(8), 1597-1603.
- Hallén, A., & Ekstrand, J. (2014). Return to play following muscle injuries in professional footballers. Journal of sports sciences, 32(13), 1229-1236.
- Wong, S., Ning, A., Lee, C., & Feeley, B. T. (2015). Return to sport after muscle injury. Current reviews in musculoskeletal medicine, 8(2), 168-175.
- Brukner, P. (2015). Hamstring injuries: prevention and treatment—an update. Br J Sports Med, 49(19), 1241-1244.

